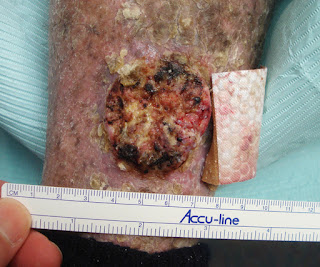
Abstract: 63 yo man with 10 month history of intense pruritus and excoriated papules and nodules
HPI: This 63 yo retired radio announcer presents with a 10 month history of intense pruritus and excoriated papules and nodules. He is in reasonable health. Medications include Welbutrin (bupropion) and occasional prednisone for his itching. He's tried topical steroids and anti-histamines without relief. Smokes ~ 5 cigarettes a day.
O/E: Skin thin from actinic damage. There are excoriated papules and nodules on the torso and extremities. There are two or three more exophytic lesions.
Clinical Photos:
Lab: CBC, chemistries normal. IgE 867 IU/Ml
Pathology: Initial bx signed out as SCC. Since he has scores of lesions repeat biopsies of an early and more developed lesion were taken. Thanks to Dr. Lynne Goldberg (Boston University Skin Path) for the beautiful photomics.
Prurigo Nodularis
Well_differentiated Squamous Cell Carcinoma
Diagnosis: Prurigo Nodularis with Squamous Cell Carcinoma
Discussion and Questions:The association of SCC with Prurigo Nodularis has only been reported one time (ref 5). Yet we do not feel this is a chance association. There are also some articles about P.n. and KA in the literature.
Has anyone seen a similar case? He will be treated with gabapentin and followed. A follow-up will be posted in a month or so. The SCCs will not be re:excised at this time.
Thaldomide has been recommended for P.N. in the literature, however, it is now > $10,000 per month!
References:
1. Journal of the American
Academy of Dermatology
Volume 69, Issue 3, Pages
426-430, September 2013
Keratoacanthomas arising in association with prurigo
nodules in pruritic, actinically damaged skin
Timothy P. Wu, BA, Kristen
Miller, MD, David E. Cohen, MD, Jennifer A. Stein, MD, PhD jennifer.Stein@nyumc.org
2. J Clin Pharm Ther. 2013
Feb;38(1):16-8. doi: 10.1111/jcpt.12005. Epub 2012 Sep 26.
Treatment of prurigo nodularis with pregabalin.
Mazza M, Guerriero G, Marano
G, Janiri L, Bria P, Mazza S.
3. Dermatol Ther. 2010
Mar-Apr;23(2):194-8. doi: 10.1111/j.1529-8019.2010.01314.x.
Therapeutic hotline: Treatment of prurigo nodularis
and lichen simplex chronicus with gabapentin.
Gencoglan G, Inanir I, Gunduz
K. (no real data on patient background)
4. Eur J Dermatol. 2008
Jan-Feb;18(1):85-6. Epub 2007 Dec 18.
Gabapentin for the treatment of recalcitrant chronic
prurigo nodularis.
Dereli T, Karaca N, Inanir I,
Oztürk G. Available Free Full Text.
5.
Saudi Med J. 2000
Mar;21(3):300-1.
Squamous cell carcinoma complicating prurigo nodularis.
Al-Waiz MM, Maluki AH.
Abstract: Squamous cell carcinoma complicating
ulcerative prurigo nodularis is described in 2 patients who were having prurigo
nodularis on dorsum of the feet for duration of many years. Biopsy specimens
from the ulcerating nodules showed features of squamous cell carcinoma. This
finding has not been previously reported. Squamous cell carcinoma should be
considered in the evaluation of long standing ulcerative lesion of prurigo
nodularis especially when not responding to conventional therapy.