Presented by Henry Foong, M.D.
Ipoh, Malaysia
The patient is a 80-year-old man who presented with swelling of the left leg for 3 months.
Ipoh, Malaysia
The patient is a 80-year-old man who presented with swelling of the left leg for 3 months.
About 3 years ago he had a motor vehicle accident where he injured his left leg. His attending doctor noticed a pigmented growth on the left foot associated with inguinal node swelling. A surgeon excised the pigmented growth on the left foot and removed some nodes from the left groin. No histological reports were available at the moment. The patient was well until recently when he noticed gradual swelling of the left leg with multiple pigmented nodules on the surface. The leg was occasionally painful at night. He did not have any constitutional symptoms. There was no family history of skin cancers. No significant other medical illness.
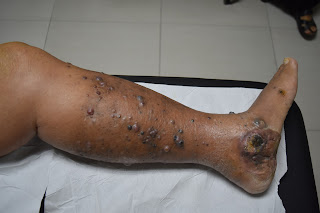
On examination his left leg was swollen and oedematous with many pigmented papules and nodules on the foot and lower 1/3 of the left leg. A pigmented ulcerating tumour 5 x 5 cm was noted on the left foot which extended to the heel. A firm matted lymph node swelling was noted on the left groin. There was a surgical scar over the left groin. No hepatosplenomegaly was present.
Biopsy of the pigmented papule on the foot was done and confirmed malignant melanoma.
Sheets and nests of malignant cells are seen invading the dermis. The tumour cells show marked pleomorphism, have increased nucleo-cytoplasmic ratio, vesicular nuclei with prominent nucleoli and eosinophilic cytoplasm. Many of the cells contain melanin pigment. Numerous mitotic figures are seen. The tumour is seen at the margins. Masson Fontana stain is focally positive.
Skin biopsy Report: Features are consistent with malignant melanoma.
On examination his left leg was swollen and oedematous with many pigmented papules and nodules on the foot and lower 1/3 of the left leg. A pigmented ulcerating tumour 5 x 5 cm was noted on the left foot which extended to the heel. A firm matted lymph node swelling was noted on the left groin. There was a surgical scar over the left groin. No hepatosplenomegaly was present.
Biopsy of the pigmented papule on the foot was done and confirmed malignant melanoma.
Sheets and nests of malignant cells are seen invading the dermis. The tumour cells show marked pleomorphism, have increased nucleo-cytoplasmic ratio, vesicular nuclei with prominent nucleoli and eosinophilic cytoplasm. Many of the cells contain melanin pigment. Numerous mitotic figures are seen. The tumour is seen at the margins. Masson Fontana stain is focally positive.
Skin biopsy Report: Features are consistent with malignant melanoma.
His work up included an oncology referral. CT scan of abdomen and pelvis which showed pelvic and para-aortic lymph
node metastasis. CXR normal. TWBC was 16,400. BRAF gene mutation studies pending
He was being treated for concomitant cellulitis with IV antibiotics.
Questions: What are the treatment options (targeted therapy) for his metastatic melanoma? Would oral vemurafenib and Anti PD-1 antibodies e.g. pembrolizumab be useful? They are very expensive though for most patients in Malaysia.
It's almost certain this patient will probably opt for palliative treatment. What local treatment of the in-trasit metastasis would be useful for him?
Thank you for your thoughts!