The patient is a 65 yo man who came in for a dermatitis of
his scalp. He requested a complete skin
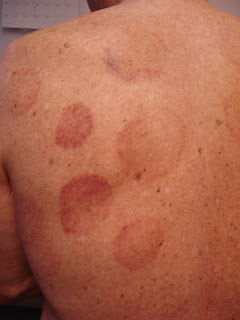
exam This was remarkable for circular
ecchymoses on his left back. I asked
about this. He sees a massage therapist
for back pain and she recommended cupping.
His wife was horrified to see these bruises until he explained how they were acquired.
Clinical Image:
With cupping, traditionally, a cotton ball soaked in alcohol
is burned inside the glass cup and removed right before placement to create the
vacuum. Bamboo and other materials can be used as alternatives to glass. The
procedure breaks superficial blood vessels in the papillary dermis, creating
ecchymoses, purpura, and petechiae, which is seen as evidence that the ailment
is being drawn from the body.
Clearly, this traditional Asian remedy is entering the
mainstream in Western Massachusetts. Our Asian readers probably see this all the time.
For a few laughs, see Cupping Video.
For a few laughs, see Cupping Video.
Reference:
1. Dermatoses caused by cultural practices: Therapeutic
cultural practices.
Vashi NA. J Am Acad Dermatol. 2018 Jul;79(1):1-16.
Abstract: With globalization and widespread immigration,
physicians increasingly encounter patients from varying backgrounds and diverse
customs. Although certain cultural practices are widely performed, there is
limited medical literature describing their dermatologic and systemic effects
and complications. Population diversity and sharing of traditions make it
increasingly important for dermatologists to understand the role of cultural
practices and recognize physiologic and pathologic sequelae. In addition,
dermatologists are often adjured to assess skin findings that may be mistaken
for abuse. Child abuse misdiagnosis can be traumatizing to all those involved,
and immigrant families with limited English proficiency may have difficulty
explaining their traditional practices. The first article of this 2-part
continuing medical education series begins with a review of therapeutic
cultural practices, including traditional Chinese medicine, Ayurveda,
acupuncture, cupping, moxibustion, and coining, and the clinically relevant
complications that may occur. Therapeutic practices can cause a range of
complications, including contact dermatitis, heavy metal toxicity, and severe
cutaneous adverse reactions.