Presented by
Tucker Slingerland, M.D. Chief Resident in Family Practice at the University of Vermont.
HPI: A 76 year old woman with multiple medical problems including chronic
hemodialysis, hypertension,
hypertriglyceridemia, and type II diabetes
mellitus presents for a second opinion on
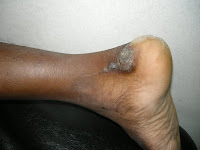
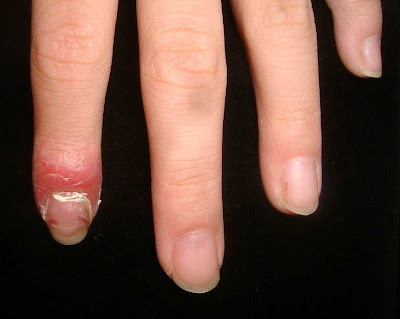
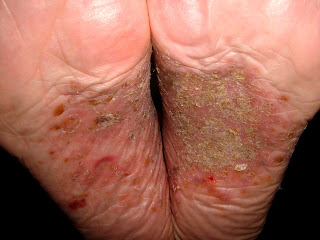
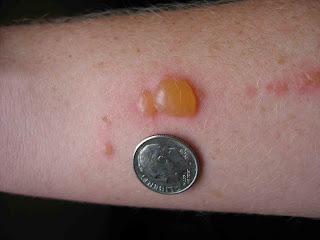
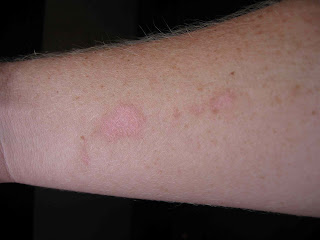
bullous lesions involving the dorsal hands, fingers, tips of ears and scalp. She had been told she had "
porphyria," given sparse information about her condition, and started on a course of
cloroquine with questionable effect.
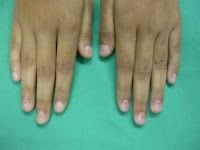
O/E: There are healing erosions on the dorsae of both hands. At this time, no bullae.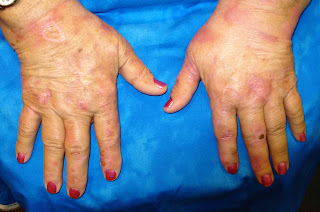
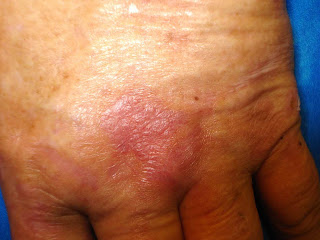
Labs and Biopsies: These were not sent to us
Discussion:A literature review using key words
porphyria cutanea tarda (PCT) and dialysis yielded a useful case report published in J Am
Acad Dermatology 2000 by
Shieh et al.(1) As reviewed in the case report, PCT is most commonly an acquired condition due to hepatic injury secondary to toxins (including drugs), hepatitis C, HIV, and
hemochromatosis which leads to a defect in heme
biosynthesis with resulting increase in iron stores (
ferritin) and
porphyrins. These
porphyrins cause
photosensitivity particularly on the
dorsae of the hands. With increasing numbers of patients with chronic renal
insufficiency on maintenance
hemodialysis, recent case reports estimate a PCT prevalence of 1.2-18% .
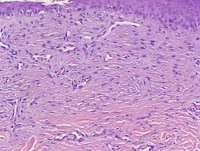
A clinical diagnosis can be confirmed with a
porphrin profile (serum, urine, fecal), skin biopsy findings detecting a
subepidermal vesicle with little inflammation, and
immunofluorescence studies. Urine tests may be difficult in the dialysis patient with little or no urine output. Serum iron studies, which are non specific but easier to obtain, will usually reflect high iron stores.
The diagnosis PCT requires excluding
pseudoporphyria (PP), a condition also consisting of
photocutaneous bullous lesions. PP can occur following sun exposure in patients who take known
photosensitizing agents such as
furosemide, 5-
flurouracil,
flutamide,
isotretinoin,
tetracycline, and
naprosyn. The key to differentiating PP from PCT is that PP occurs
without a significant increase in plasma, urinary, or fecal
porphyrins. There have also been cases of
hemodialysis associated
pseudoporphyria; further
emphasizing a need for
laboratory confirmation in our case. (2)
In patients with PCT in the
absence of renal failure, phlebotomy 250-500 ml 1-2 times per week) to decrease iron stores and
antimalarials (chloroquine
chelates porphyrins, makes them water soluble thereby allowing renal excretion) is the treatment of choice. Since chronic renal failure often coexists with chronic and sometimes severe anemia, high dose
erythropoeitin (more than 150 U/kg 3 times a week) along with careful, very small volume phlebotomy (100 ml weekly) may be a promising option as reported in at least three case reports.
In contrast, case reports of PP in the setting of
ESRD/dialysis suggest an easier treatment option having reported good results with the use of oral n-
acetylcysteine (
mucomyst).
The management of PCT in patients with renal failure is clearly a challenge that requires careful attention to other medications (avoidance of iron supplementation), frequent lab tests to help judge phlebotomy amounts and
erythropoeitin dosage, and continued patient education. For these reasons, a team approach would be ideal.
Take Home Messages:
Bullae on the dorsum of the hands, especially those that heal slowly are pathognomonic for PCT or PP. They can also be seen in phytophotocontact dermatitis from the psoralen related compounds in certain plants (especially limes and lemons that are squeezed for drinks.) Recognizing this sign will lead one to the correct diagnosis.
References:
1.
Shieh S, Cohen
JL,
Lim HW. Management of
porphyria cutanea tarda in the setting of chronic renal failure: a case report and review. J Am
Acad Dermatol. 2000 Apr;42(4):645-52.
The treatment of
porphyria cutanea tarda (PCT) in patients with chronic renal failure poses a therapeutic challenge. In the absence of renal failure, phlebotomy and oral
antimalarials have been the standard of care for PCT. However, in the presence of renal failure, associated chronic anemia often precludes the use of phlebotomy, and oral
antimalarials are usually ineffective. We describe a patient with severe symptomatic PCT and chronic renal failure whose disease was successfully managed with a combination of high-dose
erythropoietin and small volume phlebotomy. We also review several previously reported approaches to management of PCT in the setting of renal failure, which include small repeated phlebotomy,
erythropoietin,
deferoxamine, chloroquine, plasma exchange, high-efficiency/high-flux
hemodialysis,
cholestyramine, charcoal
hemoperfusion, and kidney transplantation. An algorithm for the management of these patients is proposed.
2. N. S. Cooke, K.
McKenna. A case of
haemodialysis-associated
pseudoporphyria successfully treated with oral N-
acetylcysteine. Clinical and Experimental Dermatology 32, 64–66. (2007)
We report a 33-year-old woman with
haemodialysis-associated pseudoporphyria successfully responding to treatment with oral N-acetylcysteine. We briefly review the current literature on bullous skin disorders in end-stage renal disease, and compare and contrast the pathogenesis of pseudoporphyria and porphyria cutanea tarda in this context. We also discuss the antioxidant properties and clinical applications of N-acetylcysteine, including the treatment of haemodialysis-associated pseudoporphyria.
3. A good review of PCT appears at: Emedicne/PCT but is not helpful for a patient with PCT and hemodialysis.
4. A good reference on pseudoporphyria
5. Valuable chapter on Bullous Disease of Diabetes