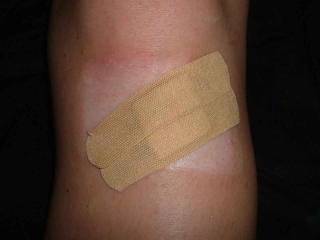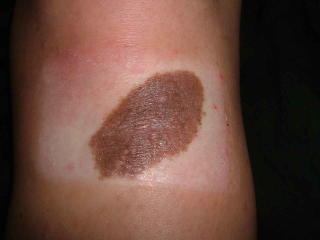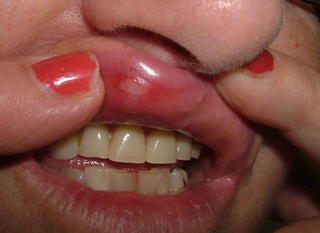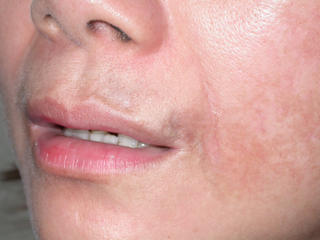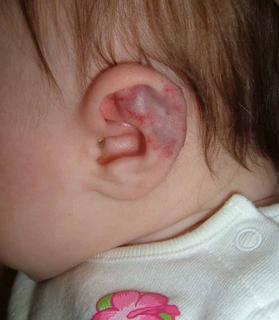
This 4 month infant girl was born with hemangiomas of the chin and left ear.
The lesion on the chin (not pictured) measures 1 cm in diameter and is typical of a congenital hemangioma.
The abnormality of the left ear involves the triangular fossa and the helix. I am concerned that as this involutes it could cause disfigurement. At the same time, I wonder if anyone has experience handling similar lesions in this site. A PubMed site found only a paucity of pertinent references.
Ref:
Cavernous hemangioma of the external ear canal.
Reeck JB, Yen TL, Szmit A, Cheung SW.
Laryngoscope. 2002 Oct;112(10):1750-2. Related Articles, Links
Division of Otology, Neurotology and Skull Base Surgery, Department of Otolaryngology-Head and Neck Surgery, Veterans Administration Medical Center, San Francisco, California, USA.
OBJECTIVE: To document the occurrence of a cavernous hemangioma of the external ear canal and to review the relevant literature.STUDY DESIGN Case report and literature review. METHODS: Review of a patient chart, imaging studies, operative report, and histologic findings. RESULTS: A cavernous hemangioma of the external ear canal not involving the tympanic membrane was surgically excised without complication. This is the third documented cavernous hemangioma of the external ear canal without tympanic membrane involvement in the English literature. Computed tomography scan is invaluable to narrow the differential diagnosis. Complete removal is curative. CONCLUSIONS: Cavernous hemangioma of the external ear canal with or without tympanic membrane involvement is a rare otologic entity amenable to surgical treatment. Temporal bone computed tomography scan imaging is an important preoperative diagnostic tool.