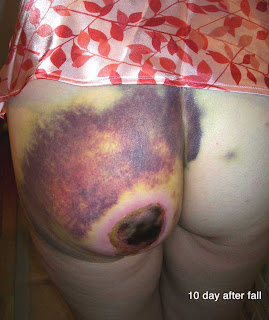
"On June 28th I fell off of my horse. Large dark hematomas covered left buttocks cheek, vagina, and coccyx. Per doctors orders warm, moist heat applied. Thw first picture, taken by my daughter ten days after the fall, shows where the circular area of skin fell off as a result of the compress. I then applied collagenase santyl cream for two weeks but was still unable to debride. One month later, in addition to area on left cheek, new symptoms have arrived which include headaches, 10 - 15 pound weight loss due to diarrhea, burning sensation in face and ears, chest pain, pain between shoulder blades and in neck. There are currently blood tests being done to confirm the existence of what is believed to be a blood disorder. [CBC and Comprehensive chem profile normal except for a slightly elevated BUN of 24 mg%]
O/E: I know this patient well as a care giver and was surprised to see how thin and pale she looked. There is a 9 cm escar on the left buttock. The tissue is necrotic and can not be debrided at this time.
Lab: A culture of the exudate under the eschar grew out many Pseudomonas aeroginosa -- sensitive to Cipro and levofloxacillin.

Discussion:
The trauma seems to have caused skin necrosis. Pseudomonas may be related as well since this looks like echthyma gangrenosum, but the patient has a presumably normal immune system and feels well otherwise. It's unclear if there was fat or muscle necrosis in addition or whether there was a compartment syndrome. The patient is now going to a wound clinic where she can get this are properly debrided.
I have not seen necrosis like this from trauma before. Similar (but more irregular necrosis) can follow brown recluse spider bite. Here, I suspect trauma was the cause; however at one month out the patient has systemic symptoms. One wonders if a CT of the buttock might be of any value.
One week later:
Wound started to drain and was explored at wound clinic. A large cavity was found under the gluteus maximus muscle (around seven cm in diameter). it was irrigated and packed. I am not sure if the cavity contained blood or pus. Today, it was clean with no drainage. The area will likely need surgical intervention as it will take months to heal by the appearance. We will seek surgical opinions.



