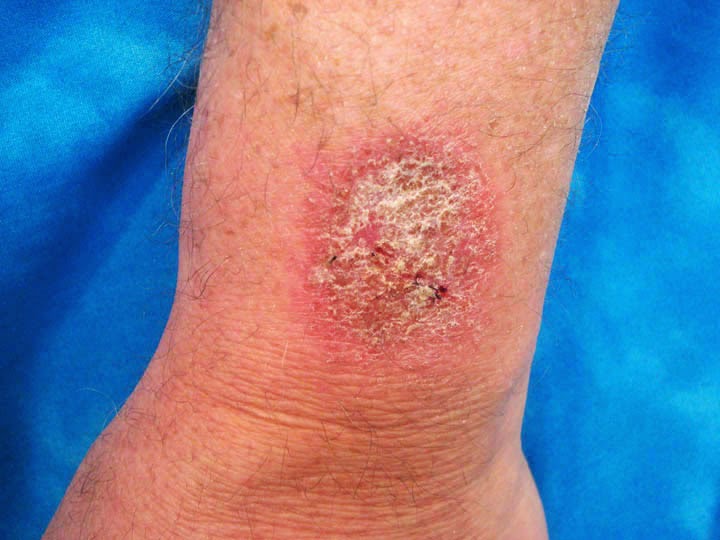
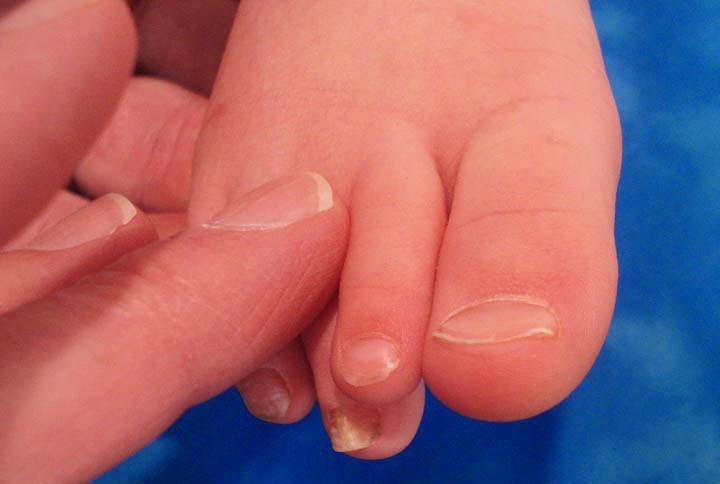
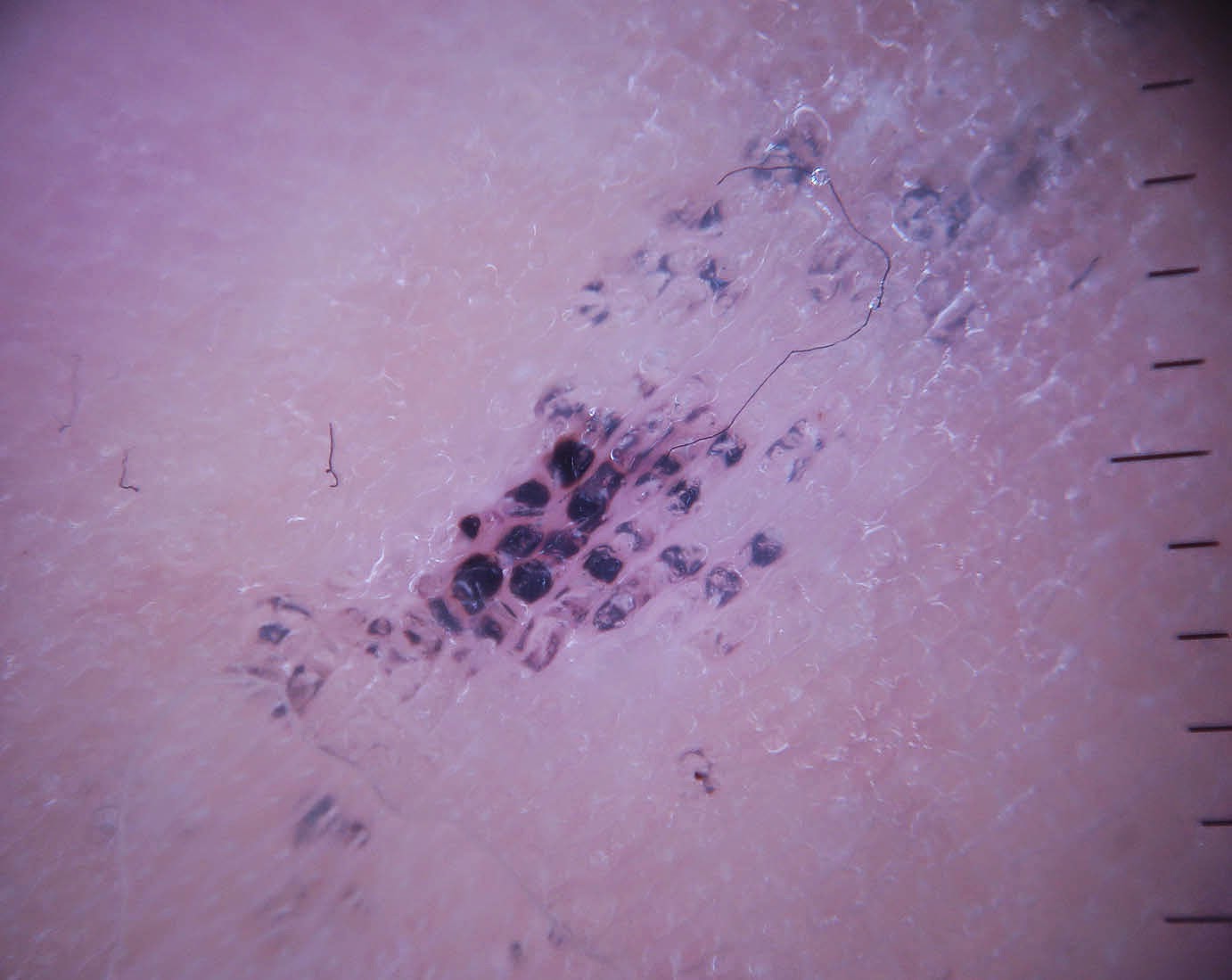
This is the history of a ftm transgendered man with relatively
early androgenetic alopecia. In spite of
his exogenous testosterone, the frontal hairline is preserved. Most of the alopecia is in parietal and
vertex areas. There is only one PubMed
reference that is pertinent, and that is not available full text.(1)
I am
a ftm Transman. I started my transition December 2013 and have been on
testosterone for about 1 year and 4 months. My resources are limited. I
have been a queer female all my life, and as a result of this, economically
marginal. I am very serious about my transition to male,. I realize that gender
is a fluid spectrum and that I am not yet sure how I will finally present as
male.
I have just turned 60 years old, though I look about 20 years younger. I have
been very athletic and have always eaten healthfully and have taken care of
myself. Perhaps this is because,
subconsciously, I knew that I would have to venture into gender transition at
some point, and thus prepared myself.
I am a musician and performer with disabling social anxieties and gender
dysphoria. This has severely hampered my ability to perform. My appearance, as
an artist, and someone who must go before the public, is a critical issue for
me. My biggest problem with transition at present is that I am beginning to
bald on the vertex of my head. If this continues unabated, I will wind up with
the typical horseshoe pate of male pattern balding.
None
of the men in my family, on either side, have this type of balding. Yes they
have receding hairlines on my father's side. Thus, I do think my particular
balding (and its rapidity) is impacted greatly by the effect of the testosterone.
This is a very disturbing and unwanted consequence of testosterone injections.
In general, I want to use testosterone for my transition, but I do not
want to be used by testosterone. I don't accept the assessment, “well at your
age, men bald.” That does not fly with me. I want to know what my options are
proactively. I have done extensive research on the Internet in regards to
balding. I have spent a lot of money trying a number of natural DHT blockers.
The problem with this, as with Propecia, is that they work by consequence of
increasing female hormones, which is unwanted in ftm transition, and also,
block facial hair, a secondary sexual characteristic very important for most
trans guys. Secondly, it is not even clear that they work to prevent balding.
Presently, I have started to use Rogaine 5% foam (just this week, so the jury
is out). Currently, I am switching my
health care to a clinic that specializes in transgenders individuals. That way,
I can also evaluate my balding in terms of testosterone levels. The
endocrinologist I see presently is not skilled enough in this regard.
I am extremely interested in any research or techniques that can be offered to
me to prevent my balding and turn it around. I am doing all I can on my own at
present, but feel there are other options and knowledge out there to which I
haven't access.
I am not out to my family yet regarding my transition to male. My appearance,
and the quality of my appearance is very personally important to my journey as
a man and to my profession as a public performer. I need to continue to be
healthy, and to look good. I want to cure my gender dysphoria so that I
can have a life. I do not want to create more obstacles blocking my success in
life.
It
has been a difficult journey! And, I am willing to do all I can. Unfortunately,
I am not in an economic position to do all I could otherwise. I do not want
this to be a limitation to my successful transition. Thus, I am seeking all
the support and help I can possibly get in relation to a truly successful transition,
unlimited by my financial circumstances. I cannot adequately express my
gratitude for any help on this challenging crossing. Any benefit I receive in these ways are not
only for myself, but will be knowledge freely disseminated, for the use of all
transmen now and in the future.
Reference:
1) Short- and long-term clinical skin effects of
testosterone treatment in trans men. Wierckx K, et al. J Sex Med. 2014 Jan;11(1):222-9.
Testosterone
(T) treatment increased facial and body hair in a
time-dependent manner. The prevalence and severity of acne in the majority of
trans men peaked 6 months after beginning T therapy. Severe skin problems were
absent after short- and long-term T treatment.
PubMed.