The patient is an otherwise healthy 62 yo man with an eight month history of an anympromatic plaque on his right arm. His work takes him to places like the Atacama desert of Chile, Baghdad and Mosul, Japan, and Indonesia where he repairs specialized equipment in the field. He was treated in a number of clinics with prednisone, various topical azoles and 40 days of grizeofulvin to no effect.
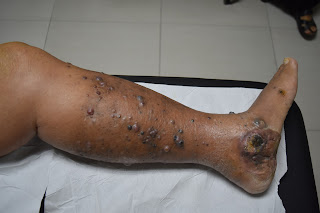
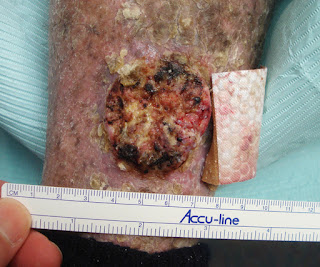
O/E: The is a solitary 10 cm ring-shaped plaque on the right arm. Sensaton to pinprick is normal.
Clinical Image:
Pathology: A 4 mm punch biopsy was taken from the border of the ring.
The
specimen exhibits a superficial and deep interstitial proliferation of
variably plump to spindle-shaped cells with mildly increased dermal
mucin and a superficial and deep perivascular lymphocytic infiltrate
with occasional plasma cells. The findings support the diagnosis of Interstitial Granulomatous Dermnatitis associated with a systemic disease.
Diagnosis: Interstitial Granulomatous Dermnatitis (IGH) vs. Granuloma annulare.
The patient lives in an endemic region for Lyme disease. His work takes him to Asia, South America, the Mid-East, and all parts of North America. Presently, he is in Iraq and will have a Lyme serology when he returns. Certainly, the clinical picture could suggest erythema migrans, but an eight month history would be unusual. There are a host of case reports of IGH in association with arthritis, collagen vascular disease, inflammatory bowel disease and even Lyme disease; but they are hard to make sense of. (Guilt by association?) Although we see erythema chronicum migrans with regularity in New England, this lesion did not jump out as typical to me; but in retrospect, it could be the interface between IGH, GA and ECM. An old ECM? Food for thought. How long will the primary lesion of Lyme disease remain without treatment. Eight months seems a long time.
References:
1. The expanding spectrum of cutaneous borreliosis.
Eisendle K1, Zelger B. G Ital Dermatol Venereol. 2009
Apr;144(2):157-71.
Abstract: The known
spectrum of skin manifestations in cutaneous Lyme disease is continuously
expanding and can not be regarded as completed. Besides the classical
manifestations of cutaneous borreliosis like erythema (chronicum) migrans,
borrelial lymphocytoma and acrodermatitis chronica atrophicans evidence is
growing that at least in part also other skin manifestations, especially morphea,
lichen sclerosus and cases of cutaneous B-cell lymphoma are causally related to
infections with Borrelia. Also granuloma annulare and interstitial
granulomatous dermatitis might be partly caused by Borrelia burgdorferi or
similar strains. There are also single reports of other skin manifestations to
be associated with borrelial infections like cutaneous sarcoidosis, necrobiosis
lipoidica and necrobiotic xanthogranuloma. In addition, as the modern chameleon
of dermatology, cutaneous borreliosis, especially borrelial lymphocytoma,
mimics other skin conditions, as has been shown for erythema annulare
centrifugum or lymphocytic infiltration (Jessner Kanof) of the skin.
2. Interstitial granulomatous dermatitis: a distinct entity
with characteristic histological and clinical pattern. Peroni A et. al. Br J Dermatol. 2012 Apr;166(4):775-83.
Abstract
BACKGROUND:
Interstitial granulomatous dermatitis (IGD) is a rare
disease for which a clinical-pathological correlation is essential to establish
diagnosis.
RESULTS:
All cases showed a predominant CD68-positive macrophage
infiltrate distributed between collagen bundles of the mid- and deep dermis.
Macrophages were also surrounding degenerated collagen fibres. A few
neutrophils and/or eosinophils were also present. No vasculitis or significant
mucin deposition was observed. Of the 62 cases of IGD reported since 1993, 53
fulfilled stringent diagnostic criteria. Erythematous papules and plaques on
the trunk and proximal limbs were the dominant manifestation. Approximately 10%
of patients had cord-like lesions. More than 50% of patients with IGD had
arthralgia or arthritis, and less commonly other rheumatic disorders. Disease
duration is months to years, but long-term prognosis seems favourable.
CONCLUSIONS:
IGD is a distinct entity with a typical histological and clinical pattern. The
importance and the nature of the association with extracutaneous diseases
remains to be clarified. Patients should be screened for rheumatic and
autoimmune diseases.
3. Erythema migrans: a spectrum of histopathologic changes.
Wilson TC et. al. Am J Dermatopathol. 2012 Dec;34(8):834-7.
Abstract: Early cutaneous Lyme disease, erythema migrans,
manifests as a gyrate erythema at the site of a tick bite. The standard
histopathologic description is that of a superficial and deep perivascular
lymphocytic infiltrate in which plasma cells are identified at the periphery of
the lesion and eosinophils in the center. Deviation from these commonly
accepted histopathologic findings may lead to an erroneous diagnosis. Herein,
we describe 4 cases of erythema migrans, all biopsied at the periphery of the
lesion and confirmed by serologic studies, demonstrating a variety of
unconventional histopathologic patterns. These findings include eosinophils and
neutrophils at the periphery of the expanding annular plaque of erythema
migrans, focal interface change, spongiosis, involvement of the superficial
vascular plexus alone, and an absence of plasma cells in all cases. These cases
highlight the varied and nonspecific histopathologic changes that can be seen
in erythema migrans, including the absence of plasma cells and the presence of
focal interface change. Based on these findings, the dermatopathologist should
always consider erythema migrans as a diagnostic possibility in a biopsy
specimen from an expanding gyrate or annular erythema despite the presence of
unusual features. In atypical clinical cases, serologic confirmation may be
required for diagnosis in the presence of histopathologic findings considered
unconventional for erythema migrans.