The patient is a 27 yo woman with a 2 week history of an
evolving, wide-spread eruption. The
initial lesions were on the popliteal fossae.
These were described as erythematous areas studded with pustules. Over a week or two these generalized. She has a history of mild psoriasis (scalp
and elbows) for over a decade. About
three months ago she was started on bupropion
75 mg a day for anxiety and restlessness. This was
increased to 150 mg per day ~ 2 week before the onset of the dermatitis. The patient has moderate cognitive impairment
and Type 2 diabetes. Here other
medications include thyroid supplementation, metformin and insulin. In the days since her initial office visit, the eruption has become more extensive and is taking on an erythrodermic appearance. She was admitted to hospital two days after her office appointment.
O/E: When seen on May 7, 2018, she had a
widespread eruption on arms, legs and torso,
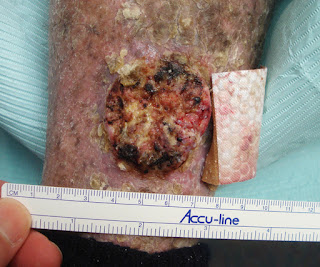
The lesions were large arcuate patches with pustules at the periphery. She was experiencing considerable pain.
Clinical
Images:
Pathology: (courtesy of DR. Erin Tababa, Fellow in Dermatology, Boston University)
Lab:
The biopsy shows prominent, relatively large, subcorneal
pustules that are filled with a dense exudate of acute inflammatory. The
neutrophils extended into the underlying epidermis, which has evidence of
mild spongiosis. The papillary dermis is slightly oedematous, and there is a
moderately dense perivascular inflammatory infiltrate with a predominance of
neutrophils, although no eosinophils are noted.
Lab:
WBC:
29,000
Differential: Shift to left
Eosinophils:
normal
G6PD Normal
G6PD Normal
Chemistries
normal.
Wound
Culture: Pending
Dx: We are initially considering subcorneal pustulr dermatosis, but with more history, especially considering the recent prescription of bupropion a drug-induced annular
pustular psoriasis evolving into pustular and exanthematous psoriasis seemed more accurate. Histopathology supported that. Similar reactions have been reported to bupropion. Our patient had been on the bupropion for over a month when this began which is longer than the patients in the case report below. Reference 2 is a similar patient with a long latent period between initiation of drug and development of GPP.
Follow-up in hospital. The eruption continued to evolve. It became more exanthematous and desquamative. These pictures were sent us by her mother.
Follow-up in hospital. The eruption continued to evolve. It became more exanthematous and desquamative. These pictures were sent us by her mother.
Plan:
Cyclosporin
3 – 4 mg per kg per day in divided doses
Wet
dressings followed by triamcinolone 0.1% ointment bid – tid
Adjunctive
secukinumab has been reported to be effective.
Follow-up:
Patient is doing very well. These photos were taken 5 days after starting cyclosporine 100 gm q.i.d. Her dose was dropped to 100 mg t.i.d. She also was treated with wet dressings and triamcinalone ointment 0.1% (although the hospital only gave her 15 mg tubes, so she could not cover most ot the lesions.
References:
Follow-up:
Patient is doing very well. These photos were taken 5 days after starting cyclosporine 100 gm q.i.d. Her dose was dropped to 100 mg t.i.d. She also was treated with wet dressings and triamcinalone ointment 0.1% (although the hospital only gave her 15 mg tubes, so she could not cover most ot the lesions.
References:
1. Generalized pustular and erythrodermic psoriasis associated
with bupropion treatment. Cox NH, Gordon PM, Dodd H. Br J Dermatol. 2002
Jun;146(6):1061-3.
Abstract: Severe drug eruptions may cause diagnostic and
therapeutic difficulty when they mimic or provoke endogenous patterns of
dermatosis. We report three patients with known psoriasis in whom use of
bupropion (Zyban), prescribed to assist with cessation of smoking, led to
severe pustular or erythrodermic exacerbation of psoriasis within 3-5 weeks.
All patients were systemically unwell and required hospitalization to control
the disease flare.
.
2. A diagnostic challenge: acute generalized exanthematous
pustulosis or pustular psoriasis due to terbinafine
L. Duckworth et.al. Clin Exp Dermatol. 2012 Jan;37(1):24-7
Abstract: A
72-year-old man developed a generalized erythematous pustular eruption 11 weeks
after commencing terbinafine. Clinically and histologically, the appearance was
that of acute generalized exanthematous pustulosis (AGEP), and the disease was
managed with topical preparations. Initial improvement was marred by relapse of
acute pustulosis, now more in keeping with terbinafine-induced pustular
psoriasis (PP),which was successfully treated with acitretin. This case highlights
the difficulty of differentiating between AGEP and PP.
3. Acute generalized exanthematous pustulosis mimicking
toxic epidermal necrolysis in patients with psoriasis: a coincidence?
Worsnop F, et. a. Clin Exp Dermatol. 2015 Aug;40(6):688-9