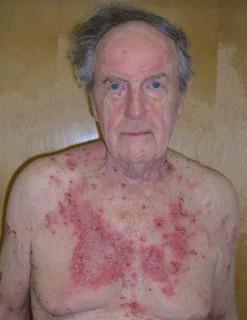
This 72 yo man had a laparoscopic cholecystectomy four months ago in Florida. Within a few weeks, he developed a bullous eruption around the area of surgery. His surgeon and primary care physician have treated with cephalosporins, topical mupirocin and triamcinalone cream. All without avail.
A culture obtained at my office showed: coagulase negative staph resistant to everything except tetracyclines and rifampin. This is probably not significant.
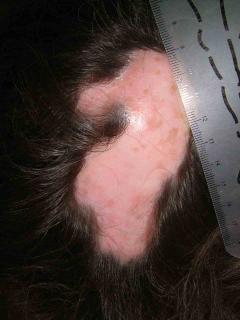
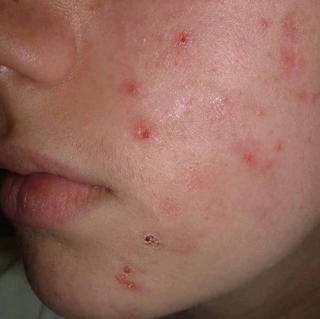
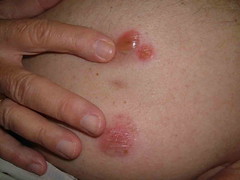
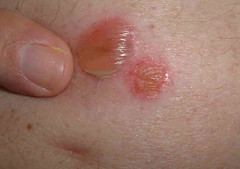
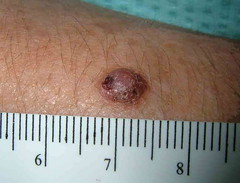
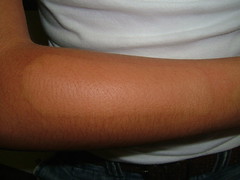
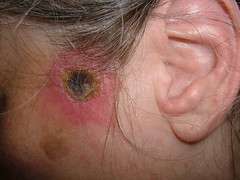
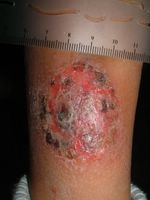
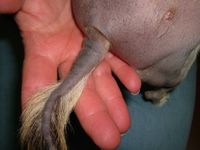
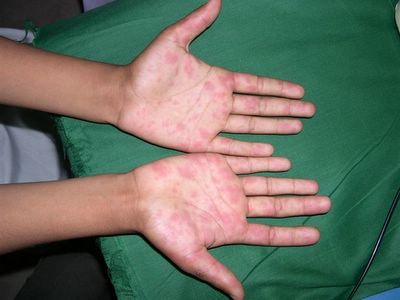
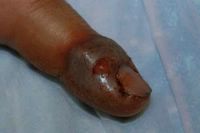
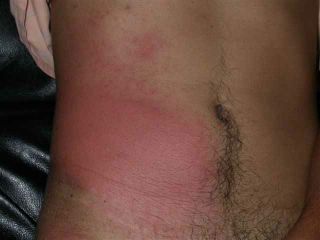
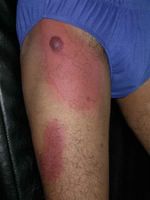
The exam shows flaccid bullae, some with fluid levels of pus. See photos of right subcostal area.
I suspect this is a localized variant of pemphigus that followed surgical trauma.
A biopsy for DIF is planned.
Is there any value iin IIF?
I started him on minocycline for the staph on the odd chance that this is an unusual pathogenic coag negative staph; but the more I think about this, themore convinced I am that this is a benign variant of P.V.
I may start superpotent topical corticosteroids since the disease manisfestation is so localized.
Not sure if localized PV has been described after laparascopic surgery.
Note laparoscopy scar between two bullae
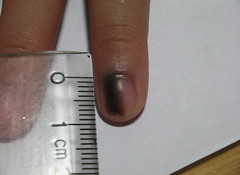
Note fluid level of wbcs
Pathology
DIAGNOSIS: Skin - (A) Abdomen:
Intra-and sub-epidermal blister with numerous eosinophils , focal re-epithelialization, eosinophil ic spongiosis and mild s uperficial perivascular lymphocytic infiltrate with numerous eosinophils and papillary dermal fibrosis .
NOTE : These findings are suggestive of re-epithelialized bullous pemphigoid . The differential diagnosis includes a bullous arthropod bite reaction or bullous drug eruption . These are not the changes of pemphigus vulgaris.
DIRECT IMMUNOFLUORESCENCE RESULTS : Perilesional skin sections were incubated with 1:10-1:20 dilutions of antisera specific for IgG, IgM, IgA and C3. "Immunostaining" was not observed.
NOTE : These findings do not support the diagnosis of bullous pemphigoid ; however, they do not exclude it as some rare cases may be negative for these immunoreactants. I f the clinical suspicion persists, an additional biopsy may be of help . Clinico-pathologic correlation is suggested.
Reference:
J Am Acad Dermatol. 1989 Mar;20(3):437-40
Direct immunofluorescence in bullous pemphigoid: effects of extent and location of lesions.
Weigand DA, Clements MK.
Dermatology Service, Veterans Administration Medical Center, Oklahoma City, OK.
We have reevaluated the previously reported conclusion that direct immunofluorescence in bullous pemphigoid is often negative in biopsy specimens from the legs. Duplicate tests from the trunk and legs were generally of equal intensity in a prospectively evaluated series of eight patients with generalized bullous pemphigoid. Also, in 36 patients evaluated retrospectively, the intensity of the direct immunofluorescence reaction correlated roughly with extent of disease, rather than with specific anatomic region. Localized disease predictably required less vigorous treatment to achieve control, but the intensity of the immunofluorescence reaction was not similarly predictive. Direct immunofluorescence is a less useful diagnostic test in localized bullous pemphigoid than in generalized bullous pemphigoid.