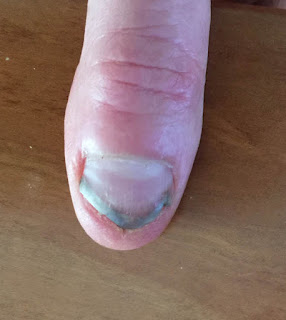
Isolated Nail Dystrophy - Left Thumb
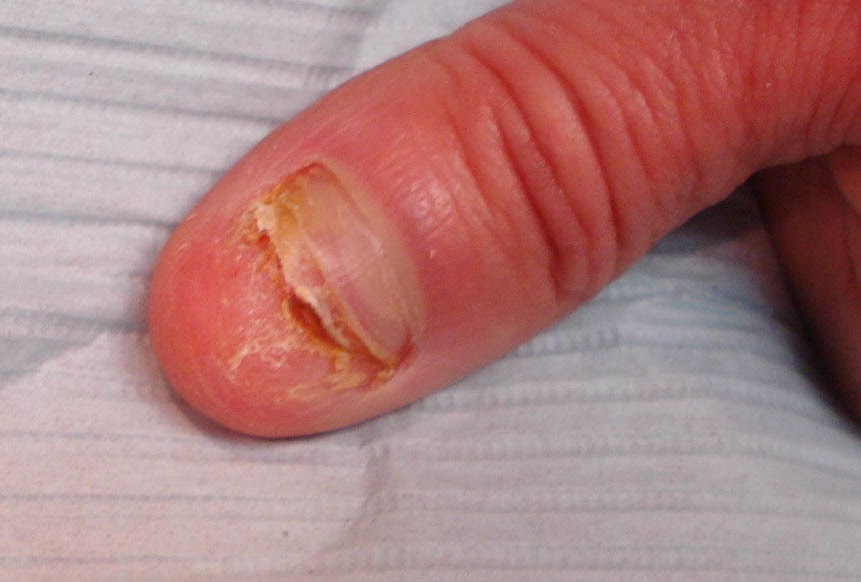 |
| My Nail 2 March 2015 |
"I’m not sure exactly how I damaged my nail, but it happened in May 2014 when I was working outdoors clearing brush. Either I banged it really hard or dropped something on it. It never really hurt, but it quickly became unsightly, with lots of bruising, mottling from black to deep mahogany to orange to yellow. The nail developed a significant ridge until October 2014, when it came off in one piece.
Underneath was what you saw pictured above, a partial nail that is quite horny and yellow on the lower right and not tightly attached; it seems to grow outward rather than lie flat. I had an acrylic nail put on when I had to be very public for a couple of weeks; otherwise I’ve mainly kept a bandaid over it so that I won’t keep hitting it and also because it’s so ugly."
Note: A KOH scraping was negative and fungal culture was taken.
Six month Follow-up.
The culture grew out (Scopulariopsis), a saprophytic fungus and the patient has been using topical Tea Tree oil. There has been marked improvement. We recommend continued conservative management. The nail did not continue to do well and the patient took terbinafine 250 mg a day for 3 month (no benefit).
January 2017
The patient's nail now shows signs of onycholysis. It now has a green color indicative of "chloronychia." This is probably psudomonas. She has had a nail dystrophy now for ~ two years. I think probably best to treat for pseudomonas, but the patient is wondering if her nail should be removed.
February 24, 2017
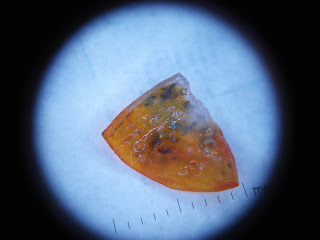 |
| Dermatoscopy of Nail Fragment |
 |
| photomic of Scopularopsis (from WWW) |
The nail was pared back.
The patient will apply 40% urea cream to the nail plate and bed and tape the surrounding area.
She will use topical gentamycin and a topical antifungal.
Pathology: PAS Stains from Nail (2.24.17) Showing fungal elements.
4.5.2017
This is the appearance six weeks after nail trimmed back which was followed up by topical gentamycin for pseudomonas, Jublia, and one pulse of itraconazole (400 mg daily for seven days) Two more pulses are planned.
6.26.17
June 26, 2017 is after three montly pulses of itraconazole (400 mg b.i.d. x 1 week/month) and daily topical efinaconazole (Jublia). We plan to keep up with the latter for another couple of months. This is the best the patient has looked in three years. She still may have a bit more to go.
Questions:
What would be the best topical antifungal available in the U.S. for this patient?
Is there a role for a different systemic antifungal, such as itraconazole? (Terbinafine was not successful)
What role does the taping play?
Reference:
1. Onychomycosis Caused by Scopulariopsis brevicaulis: Report
of Two Cases
Myung Hoon Lee, M.D., et. al. Ann Dermatol. 2012 May; 24(2):
209–213. Free Full Text.
2. Anchor Taping Method per Dr. Hiroko Arai.
2. Anchor Taping Method per Dr. Hiroko Arai.
3. Onychomycosis caused by Scopulariopsis brevicaulis: report
of two cases.
Lee MH1, Hwang SM, Suh MK, Ha GY, Kim H, Park JY. PMC Full Text
Ann Dermatol. 2012 May;24(2):209-13.
Abstract: Onychomycosis is usually caused by dermatophytes,
but some nondermatophytic molds and yeasts are also associated with invasion of
nails. Scopulariopsis brevicaulis is a nondermatophytic mold found in soil as a
saprophyte. We report two cases of onychomycosis caused by S. brevicaulis in a
48-year-old male and a 79-year-old female. The two patients presented with a
typical distal and lateral subungual onychomycosis. Direct microscopic
examination of the potassium hydroxide preparation revealed fungal elements.
From toenail lesions of the patients, brown colonies with powdery surface,
which are a characteristic of S. brevicaulis, were cultured on two Sabouraud's
dextrose agar plates. Three cultures taken from nail plates within a 2-week
interval yielded similar findings. Numerous branched conidiophores with chains
of rough walled, lemon-shaped conidia were observed in slide culture by light
microscopy and scanning electron microscopy. The nucleotide sequences of the
internal transcribed spacer for the two clinical isolates were identical to
that of S. brevicaulis strain WM 04.498. To date, a total of 13 cases of S.
brevicaulis onychomycosis including the two present cases have been reported in
Korea. Mean age of the patients was 46.1 years, with a higher prevalence in
males (69.2%). Toenail involvement was observed in all cases including a case
involving both fingernail and toenail. The most frequent clinical presentation
was distal and lateral subungual onychomycosis in 12 cases, while one case was
proximal subungual onychomycosis.