This 64 yo light-complected carpenter noticed a few rough spots on his chest. Since he vacations in Mexico two to three times a years, he is worried re: skin cancer.
A skin exam showed a 4 mm nodular BCC on his chest and a few hypertrophic AKs on the chest. An incidental finding (that he was unaware of) was a 6 mm in diameter irregularly pigmented papule on the right upper back. The dermatoscopic image is ugly and worrisome.
He is scheduled for an excisional biopsy.
This case is very similar to that presented on VGRD last week. Therefore, this patient probably has a SSM that is < 1 mm thick. We will see.
Thursday, December 29, 2016
Tuesday, December 20, 2016
New Pigmented Lesion
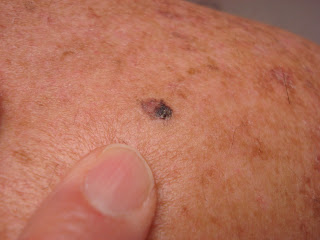
Thiss 56 year-old man was brought into the office by his wife who has noticed a new pigmentedlesion on his mid-back for around a year. He did not see the point in coming in, but she made the appointment and came in with him.
The exam showed a 1.1 cm pigmented nodule with a play of color and irregular borders. The dermatoscopic exam shows whitish areas, black areas, and pigment dots (among other things).
Clinically, I thought this was a superficially spreading melanoma. I could not be 100% sure it was not a seborrheic keratosis.
An excisional biopsy was done. Pathology will be added in a few days.
Pathology: Superficial spreading melanoma, at greatest, 0.68 mm thick.
I will recommend a WLE. Not further studies.
Note: Often, a wife will make the appointment for her husband who is reluctant to see the physician. This patient insisted on going to work as a pipe-fitter after the excision. When a wife finds a lesion on her skin and asks her husband to take a look; he often says to her, "If your worried, see a doctor."
The exam showed a 1.1 cm pigmented nodule with a play of color and irregular borders. The dermatoscopic exam shows whitish areas, black areas, and pigment dots (among other things).
Clinically, I thought this was a superficially spreading melanoma. I could not be 100% sure it was not a seborrheic keratosis.
An excisional biopsy was done. Pathology will be added in a few days.
Pathology: Superficial spreading melanoma, at greatest, 0.68 mm thick.
I will recommend a WLE. Not further studies.
Note: Often, a wife will make the appointment for her husband who is reluctant to see the physician. This patient insisted on going to work as a pipe-fitter after the excision. When a wife finds a lesion on her skin and asks her husband to take a look; he often says to her, "If your worried, see a doctor."
Thursday, December 08, 2016
A Case for Diagnosis
History: The patient is an otherwise healthy 67 year-old writer with a three month history of an intensely pruritic papular
and pustular dermatitis in an otherwise. He’s been on Welbutrin, HCTZ and Lipitor for
years. Previously treatments
with triamcinolone 0.1% ointment and prednisone for two weeks were not helpful.
O/E: There are
hundreds of 2 – 3 mm erythematous papules on arms, legs, torso, scalp. Face spared.
No lesions on hands, feet or genitalia.
Clinical Images:
Pathology:
Lab: CBC, Chemistries normal. Wound culure grew 2+ SAUR sensitive to everything.
The patient was treated with Keflex 250 mg qid for a week and Prednisone starting at 40 mg a day. He cleared quickly, but when he stopped the prednisone after ~ 3 weeks, the eruption and pruritus recurred. The new lesions are distinct erythematous papules mostly on the torso. Background looks normal.
Thoughts: Could this be "subacute prurigo" othewise known as Itchy Red Bump Disease? I will have slides reviewed and offer another biopsy to the patient.The patient was treated with Keflex 250 mg qid for a week and Prednisone starting at 40 mg a day. He cleared quickly, but when he stopped the prednisone after ~ 3 weeks, the eruption and pruritus recurred. The new lesions are distinct erythematous papules mostly on the torso. Background looks normal.
Tuesday, November 29, 2016
Cutaneous Sarcoidal Granulomas
thinking outside of the box
57 year-old woman with a one-year history of an eruption on arms and legs
This 57 y.o. woman first noticed asymptomatic, erythematous patches on
arms and legs a year ago. She is in otherwise good
health and was taking
Losartan/ HCTZ and Pravastatin for hypertension and cholesterol by mouth.
She lived in Texas for five years in the 1980s, but otherwise spent
her entire life in Western Massachusetts.
In September 2016, biopsies obtained from the right arm and
left leg showed sarcoidal granulomatous dermatitis.
Clinical:
Her skin lesions, mostly on the arms and legs, are few and scattered. They are erythematous, slightly scaly, ill-defined plaques with irregular borders.
Her skin lesions, mostly on the arms and legs, are few and scattered. They are erythematous, slightly scaly, ill-defined plaques with irregular borders.
Pathology:
Photomicrographs graphs and interpretations courtesy of Dr. Deon Wolpowitz
Boston University, Department of Dermatology
The specimen exhibits superficial and deep, nodular well-formed collections of epithelioid histiocytes and multinucleated giant cells forming granulomas with sparse to mild lymphocytic rims and a moderate superficial and mid perivascular lymphocytic infiltrate. The histologic differential diagnosis includes sarcoidosis, a foreign body reaction, and infectious etiologies including mycobacterial infections. Polariscopic examination is negative. Fite stain is negative for mycobacteria. PAS stain is negative for fungal organisms.
Lab: CBC and
chemistries were normal, as was her chest x-ray.
Discussion: This woman has
no risk factors for sarcoidosis, but did spend five years in a geographic
setting where sarcoid is more commonly seen. The only thing we came up with was that
she was using a cat litter with silica in it and there is one reference in the
literature to that being associated with sarcoidosis.
References:
1. Cat litter is a possible trigger for sarcoidosis.
Drent M, Wijnen PA, Boots AW, Bast A. Eur Respir J. 2012
Jan;39(1):221-2. Free Full Text. This is the fascinating report of a single case of
pulmonary sarcoidosis that appeared to be causally related
to silica containing kitty litter.
2.
Mahony J, Helms SE, Brodell RT. The sarcoidal granuloma: A unifying
hypothesis for an enigmatic response. Clin Dermatol. 2014 Sep-Oct; 32(5):654-9
Abstract: Although the cause of sarcoidosis is unknown,
there is growing support for the concept that sarcoidal granulomas result from
a hypersensitivity reaction producing a nonspecific response to an extrinsic or
intrinsic (autoimmune) antigen in genetically susceptible individuals. The
immune milieu associated with these antigens, localized in a specific cutaneous
area, produces a variant of Ruocco's "immunocompromised district."
This may explain the predilection for sarcoidal granulomas in association with
foreign bodies, tattoos, herpes zoster-affected dermatomes, and scars. Similar
antigenic stimulation produces sarcoidal granulomas surrounding internal
tumors. Finally, systemic sarcoidosis, as manifested by hilar adenopathy, may
reflect the lymphatic spread of foreign antigens.
Friday, October 28, 2016
Chronic Localized Folliculitis
The patient is a healthy 28 yo man with a five year history of erythematous papules and pustules on the central upper chest. No improvement over the past few years.
O/E: There are erythematous crusted papules and pustules mid upper chest. No other cutaneous lesions.
Clinical Photos:
Path: 4 mm punch bx x 2: Both specimens show a dense perifollicular neutrophilic iinfiltrate forming abscesses and infiltrating follicular epithelium with admixed lymphocytes, plasma cells and histiocytes. GMS and PAS and gram stain negative.
Deon Wolpowitz, M.D. of B.U. Skin Pathology provided these impressive microscopic photographs.
Lab: Two bacterial cultures taken from a pustules a year apart show only coagulase negative staph.
Diagnosis: Chronic Localized Folliculitis. Simplistically, I am thinking about Majocci's granuloma or an atypical form of acne.
The patient is reluctant to try isotretinoin or systemic antibiotics. He is a healthy person in all other respects and has fears about messing with is microbiome and has read about isotretinoin and is worried.
O/E: There are erythematous crusted papules and pustules mid upper chest. No other cutaneous lesions.
Clinical Photos:
Path: 4 mm punch bx x 2: Both specimens show a dense perifollicular neutrophilic iinfiltrate forming abscesses and infiltrating follicular epithelium with admixed lymphocytes, plasma cells and histiocytes. GMS and PAS and gram stain negative.
Deon Wolpowitz, M.D. of B.U. Skin Pathology provided these impressive microscopic photographs.
Lab: Two bacterial cultures taken from a pustules a year apart show only coagulase negative staph.
Diagnosis: Chronic Localized Folliculitis. Simplistically, I am thinking about Majocci's granuloma or an atypical form of acne.
The patient is reluctant to try isotretinoin or systemic antibiotics. He is a healthy person in all other respects and has fears about messing with is microbiome and has read about isotretinoin and is worried.
Thursday, October 27, 2016
Chronic Recurrent Axillary Dermatitis
Six yo old boy with > 3 year history of recurrent dermatitis
HPI: The patient is an otherwise healthy six year-old boy with a > three year history of a dermatitis in the left axilla. There is no pertinent family history. He has had similar areas since infancy. A culture taken in February 2013 showed many coag + Staph aureus. He was treated then with mupirocin ointment and betamethasone valerate 0.1% cream with good results.
O/E: Localized crusted erosions left axilla. No other lesions today.
Clinical Photos 10/31/16)
Lab: Repeat bacterial culture taken.
HPI: The patient is an otherwise healthy six year-old boy with a > three year history of a dermatitis in the left axilla. There is no pertinent family history. He has had similar areas since infancy. A culture taken in February 2013 showed many coag + Staph aureus. He was treated then with mupirocin ointment and betamethasone valerate 0.1% cream with good results.
O/E: Localized crusted erosions left axilla. No other lesions today.
Clinical Photos 10/31/16)
Lab: Repeat bacterial culture taken.
Friday, October 21, 2016
Sulzberger on Caring for Patients
Yoon Cohen sent this quotation to us. Readers of VGRD will appreciate it:
I know of no better way to start teaching a student of
medicine than by repeating over and over the old-time physician's concept of
his responsibilities toward his patients: to cure sometimes; to help often; to
comfort always.
Perhaps the most fundamental requirement to become a more
than ordinary practitioner is to be able to put yourself as wholly as possible
into the patient's place. This is not as easy to do as it sounds. I told my
young colleagues: "As you sit opposite your patient, try to think about
his or her problems so intensely that you lift yourself mentally into his
shoes, his seat, his pants, his home, his work, his problems."
They were told over and over again: "Every patient who
comes to us is in trouble. Whether the complaint seems serious or trivial to
you, it is serious to the patient and deserves your full attention and your
best efforts. You may have just seen ten patients with more grave or more
interesting skin diseases, but to the patient you are now examining, his
trouble is the most important in the world at that moment. You must be kind and
patient even with those who are over-demanding, unreasonable, even
antagonistic. Remember that those attitudes too are signs of illness and often
the results of fear, anxiety, or ignorance."
Marion B. Sulzberger
Marion B. Sulzberger
Sunday, October 09, 2016
Florid Acneiform Eruption
Presented
by:
Marina Delgado, M.D.
Apache Junction, Arizona
Marina Delgado, M.D.
Apache Junction, Arizona
The
patient, a 21 woman with a 9 year history of acne is studying in Arizona. Her acne, present since age 12, was relatively
quiescent until it flared three months ago when she was doing research in Southern
China. In the past, she had been treated with topicals, antibiotics and
oral contraceptives. None were effective; but her acne was not florid as it is now.
 |
| 10.9.2016 |
 |
| 5.12.2017 |
One of our pediatric dermatology colleagues suggested that this woman has pyoderma faciale.
We recommended isotretinoin plus prednisone but, because
of iPledge, the patient has to wait a month to qualify for isotretinoin.
Have you managed similar patients? What suggestions do you have? What do you see as the role for prednisone and how long shoould it be continued?
References:
1. Pyoderma faciale:
Successful treatment with isotretinoin
Victor J. Marks,
Robert A. Briggaman
J Am Acad Dermatol
17, 1062–106. 1987 PDF.
2. Henry Foong. Pyoderma faciale, Virtual Grant Rounds in Dermatology, October 2001.
3.
2. Henry Foong. Pyoderma faciale, Virtual Grant Rounds in Dermatology, October 2001.
3.
Combination of low-dose isotretinoin and pulsed oral
azithromycin in the management of moderate to severe acne: a preliminary
open-label, prospective, non-comparative, single-centre study. De D1, Kanwar AJ. Clin Drug Investig.
2011;31(8):599-604.
RESULTS: Sixty-two (93.9%) of 66 eligible patients had
complete clearance of disease activity after a mean treatment duration of 21
weeks. The mean total cumulative dose of isotretinoin was 49.6 mg/kg. Seven
(11.3%) patients had a relapse of disease during the post-treatment follow-up
period. Fifty-three adverse effects were observed. Three patients had initial
aggravation of disease that was managed with prednisolone and disappeared with
continuation of treatment.
CONCLUSION: A combination of low-dose isotretinoin and oral
azithromycin pulse is effective in severe acne and has a reasonably acceptable
adverse-effect profile and low post-treatment relapse rates. Abstract.
Monday, October 03, 2016
Extensive Darier's Disease
This 55 yo man
presents with a flare of Darier’s disease. In his own words, he suffers
from “mental illness” and has been on lithium for decades. He very
embarassed about his skin and feels that he looks “hideous” because of
this. Two yeas ago he had squamous cell carcinoma of the base of the
tongue that was treated with surgery, radiation and chemothreapy. This is in remission presently.
O/E: The examination shows widespread discrete and confluent reddish-brown greasy papules on the the chest and back.
We have treated him successfully with isotretinoin in the past and were concerned about the possible interaction between lithium and isotretinoin, but the patient is at his wits end with his disease.
PLAN: He was requalified for iPledge today. He will be started on 40 mg of isotretinoin a day. In a month, we will do biochemistry survey, CBC, lipid profile, and lithium level. We will obtain his last lithium level, in addition.
The patient was treated with 40 mg of isotretinoin daily. After a few months, he is completely clear and his dosage is being tapered.
References
Isotretinoin treatment of Darier's disease.
J Am Acad Dermatol. 1982 Apr;6(4 Pt 2 Suppl):721-6.
Dicken CH, et, al.
J Am Acad Dermatol. 1982 Apr;6(4 Pt 2 Suppl):721-6.
Dicken CH, et, al.
Thursday, September 22, 2016
Airborn Contact Dermatitis?
The patient is an 83 yo woman who has had a recurring pruritic dermatitis located mostly on face, neck and upper chest for two years. It seems to be more prominent seasonally. She has a history of a lymphoma ~ five years ago. She had alopecia universalis for many years that spontaneously remitted ~ two years ago.
O/E: Florid erythema of face and neck. Submental area does not appear to be spared.
This woman has a somewhat "leonine" facies.
Diagnosis: Initially, I thought she had a contact dermatitis or the "red face syndrome" from overuse of topical corticosteroids. She has been off the latter for > 1 year. The has needed prednisone to control this; but I prefer a long-term medication with less side-effects. Given her history of lymphoma, further evaluation may be necessary.
References:
O/E: Florid erythema of face and neck. Submental area does not appear to be spared.
This woman has a somewhat "leonine" facies.
Diagnosis: Initially, I thought she had a contact dermatitis or the "red face syndrome" from overuse of topical corticosteroids. She has been off the latter for > 1 year. The has needed prednisone to control this; but I prefer a long-term medication with less side-effects. Given her history of lymphoma, further evaluation may be necessary.
References:
Azathioprine versus betamethasone for the treatment of
parthenium dermatitis: a randomized controlled study.
Verma KK1, Mahesh R, Srivastava P, Ramam M, Mukhopadhyaya
AK.
Indian J Dermatol Venereol Leprol. 2008 Sep-Oct;74(5):453-7
Author information: prokverma@hotmail.com
Abstract
CONCLUSIONS: Azathioprine and betamethasone appear to be
almost equally effective (P=0.0156 vs. 0.0005) in the treatment of parthenium
dermatitis. However, adverse effects and relapses were observed to be more
frequent in patients treated with betamethasone. Free Full Text
Tuesday, September 06, 2016
Postiive Band-Aid Sign
The patient is a 77 y.o. man who presented with a number of skin lesions. He has a past history of non-melanoma skin cancer.
The lesion in question has been present for a few months. It is an almost 5 cm in diameter exophytic tumor.
Diagnosis: Probable Squamous Cell Carcinoma.
I anesthetized the lesion and shaved it off. There was a fair amount of bleeding. I curretted it and cautrized the base. It was not as soft as a typical SCC or BCC. Specimen submitted and I'll attach a follow-up with the path.
Pathology: Well-differentiated squamous cell carcinoma
This is a particularly good example of the "Positive-Band Aid" sign. Most of us know this, but it has not been well-reported in the literature. We presented this sign on the VGRD Blog in 2007.
The lesion in question has been present for a few months. It is an almost 5 cm in diameter exophytic tumor.
Diagnosis: Probable Squamous Cell Carcinoma.
I anesthetized the lesion and shaved it off. There was a fair amount of bleeding. I curretted it and cautrized the base. It was not as soft as a typical SCC or BCC. Specimen submitted and I'll attach a follow-up with the path.
Pathology: Well-differentiated squamous cell carcinoma
This is a particularly good example of the "Positive-Band Aid" sign. Most of us know this, but it has not been well-reported in the literature. We presented this sign on the VGRD Blog in 2007.
Saturday, September 03, 2016
The Tortured Tube
The patient is a 25 yo man with a 4 mo hx of an eyelid
dermatitis. His mother, a health
professional, gave him 0.1% triamcinalone oinment to apply ~ 2 months ago. It has run out and he came in for an
appointment. He is healthy and has a
history of atopic dermatitis that is now quiescent.
Diagnosis and Discussion: I think this is an example of "steroid acne." It's hard to tell what preceded it. Most topical corticosteroids when applied for weeks or more to thin skin such as is seen on the face (expecially eyelids or around the mouth) or the genitalia can cause this. It's a type of steroid addiction.
The standard treatment is to stop the topical steroid, apply cold compresses two time a day and doxycycline 100 mg b.i.d. for a month or more. The longer this has been going on, the harder it is to treat.
Reference: Dr. Ken Fowler and I reported a similar patient in 2001.
Tuesday, August 30, 2016
Linear Pruritic Lesions
Dr. Yogesh Jain would appreciate your comments about the following patient:
18 year old man with no significant past medical history, presented with these lesions to the OPD. He revealed that he has been having such lesions ever since he was 2 years of age. These excoriative lesions are very itchy, but not painful. They extends from the left groin till the medial malleolus in a continous pattern. And also involve the left arm in a similar fashion affecting the palm as well. He is not on any medications. There are no other systemic positive finding.
18 year old man with no significant past medical history, presented with these lesions to the OPD. He revealed that he has been having such lesions ever since he was 2 years of age. These excoriative lesions are very itchy, but not painful. They extends from the left groin till the medial malleolus in a continous pattern. And also involve the left arm in a similar fashion affecting the palm as well. He is not on any medications. There are no other systemic positive finding.
Wednesday, August 17, 2016
Dermatitis Neglecta
The patient is a 15 yo boy with a three month history of a dermatosis of his cheeks.
O/E: Slightly greenish symmetrical dermatosis of cheeks. Othewise, normal.
Photos taken by patient's mother and emailed to me.
Dermatoscopic images before and after area was cleansed with an alcohol pledget.
Diagnosis: Dermatitis Neglecta
There are no descriptions of the dermatoscopic appearance of this disorder.
O/E: Slightly greenish symmetrical dermatosis of cheeks. Othewise, normal.
Photos taken by patient's mother and emailed to me.
Dermatoscopic images before and after area was cleansed with an alcohol pledget.
Diagnosis: Dermatitis Neglecta
There are no descriptions of the dermatoscopic appearance of this disorder.
Saturday, August 06, 2016
Laugier Hunziker syndrome
The patient is a 74 yo man with a long history of oral
hyperpigmentation. He was presented on
VGRD in 2012, but we have further history now.
The pigmentation has been present many years. His mother had a similar
process by history.
He has a history of colon polyps. His paternal grandmother
had colon cancer. His mother had colonic polyps and breast cancer. His father
and his father’s brother both had leukemia.
O/E: There are
multiple dark brown irregular lenticular hyperpigmented macules of 2–5 mm
diameteron the lower lip ant tongue. No
other hyperpigmentation was noted.
Clinical Image:
Diagnosis: Laugier Hunziker syndrome vs Peutz Jeghers syndrome
Case to be discussed at Hot Spots 2016
References:
1. Laugier–Hunziker Syndrome: A Rare Cause of Oral and Acral
Pigmentation
Silonie Sachdeva, Shabina Sachdeva, and Pranav Kapoor
J Cutan Aesthet Surg. 2011 Jan-Apr; 4(1): 58–60.
Abstract: Laugier–Hunziker syndrome (LHS) is an acquired,
benign pigmentary skin condition involving oral cavity including lower lip in
the form of brown black macules 1–5 mm in size, frequently associated with
longitudinal melanonychia. There is no underlying systemic abnormality or
malignant predisposition associated with LHS, and therefore the prognosis is
good. Important differential diagnoses include Peutz Jeghers syndrome and
Addison’s disease among other causes of oral and acral pigmentation. PubMed Central.
Wednesday, July 13, 2016
Annular Lesions in a 50 yo woman
This image was sent by Dr. Yogesh Jain from India for diagnostic suggestions.
The only history provided was that the process is present on the hands and feet and has been ongoing for 25 years. The lesions regress after a number of months.
Other than a variant of granuloma annulare or elastosis perforans serpiginosa, what are your thoughts?
Biopsy is important but so is the dermatopathologist who reads it.
The only history provided was that the process is present on the hands and feet and has been ongoing for 25 years. The lesions regress after a number of months.
Other than a variant of granuloma annulare or elastosis perforans serpiginosa, what are your thoughts?
Biopsy is important but so is the dermatopathologist who reads it.
Saturday, July 02, 2016
What is Right Care?
The patient is a 90 year-old
man, homebound with a dementia. His 87
year-old wife is a steadfast, loving and loyal caregiver. His dermatologist has made house calls for
the past four months.
There are non-melanoma skin
cancers on the left cheek and mid upper
lip. The former lesion has increased
from 1.3 to 1.5 mm in diameter and the the lip lesion has increased from 1.8 to
2.2 mm in diameter in the past two months.
Both are somewhat inflammatory and crusted. He picks on the lip lesion,
but because of his dementia he can not articulate what it is that bothers him.
 |
| 6.28.2016 |
 |
| 8.11.16 |
A trial of topical 5-FU plus
imiquimod may be helpful, especially for the lesion on the lip, as a palliative
procedure. The lesion on the malar
eminence which grew rapidly ~ 6 months ago and is either a squamous cell or a
keratoacanthoma) could be curetted and dessicated.
The patient can not make a
decision for himself and his wife wants to just watch these lesions. She understands that treatment is not likely
impact on his quality of life at this point and want’s to spare him the trauma or surgery.
As physicians, we feel compelled
to “do something.” Is this the right
time to “not just do something, but to sit there.”
Reference:
1. Linos E. Treatment of
nonfatal conditions at the end of life: nonmelanoma skin cancer. JAMA Intern Med. 2013 Jun 10;173(11):1006-12
CONCLUSIONS AND RELEVANCE: Most
NMSCs are treated surgically, regardless of the patient's life expectancy.
Given the very low tumor recurrence rates and high mortality from causes unrelated
to NMSC in patients with limited life expectancy, clinicians should consider
whether these patients would prefer less invasive treatment strategies. PubMed. PMC Free Full Text.
2.
Knocking on Heaven’s
Door
by Katie Butler is an
honest, sobering book that describes what awaits so many elderly people and
their caregivers, who are often family members. It is relevant to how one
manages a patient such as the man described and discussed here.
Thursday, June 16, 2016
Hypopigmentation in an African
The patient is a 39 yo man from Ghana. His wife noticed these spots on his back recently. My first diagnosis was tinea versicolor; but KOH prep showed only spores. Is this just quiescent T.v.? It's symmetrically distributed over upper back (no where else). In differential diagnosis was vitiligo -- but this is incomplete hypopigmentyation (which can occur with vitiligo, but less commonly). I suggested ketoconazole cream and a follow-up in 3 months. If still present, may do a biopsy.
What are your thoughts?
References:
What are your thoughts?
References:
1.
The utility of dermoscopy in the diagnosis of evolving
lesions of vitiligo.
Thatte SS1, Khopkar US.
Indian J Dermatol Venereol Leprol. 2014 Nov-Dec;80(6):505-8.
BACKGROURD: Early lesions of vitiligo can be confused with
various other causes of hypopigmentation and depigmentation. Few workers have
utilized dermoscopy for the diagnosis of evolving lesions of vitiligo.
CONCLUSION: Pigmentary network changes, and perifollicular
and perilesional hyperpigmentation on polarized light examination, and a
diffuse white glow on ultraviolet light examination were noted in evolving
vitiligo lesions. Histopathological examination was comparatively less
reliable. Dermoscopy appears to be better than routine histopathology in the
diagnosis of evolving lesions of vitiligo and can obviate the need for a skin
biopsy. Free Full Text.
2.
Dermoscopy as an ancillary tool for the diagnosis of
pityriasis versicolor.
Zhou H, Tang XH, Chen MK. J Am Acad Dermatol. 2015
Dec;73(6):e205-6. (this is only reference in PubMed on T.v. and dermsocopy and it is not particularly helpful)
3. Dermatoscope--the dermatologist's stethoscope.
3. Dermatoscope--the dermatologist's stethoscope.
Lallas A, Argenziano G.
Indian J Dermatol Venereol Leprol. 2014 Nov-Dec;80(6):493-4. Full
Free Text
This is an interesting somewhat philosophical article. The references are extensive and helpful.
Subscribe to:
Posts (Atom)