The child appears normal otherwise. He has no evidence of atopy. This is the largest lesion. All are plaques, all covered with some crust, intensely pruritic. I applied some pressure to the large plaque with a cotton tipped applicator and a small amount of creamy pus was extruded.
My working diagnosis is nummular eczema driven by hypersensitivity to staph. A culture was taken and I'll wait for results before treating. This has been going on for 5 years. I may do a biopsy, but am not sure it will be helpful.
Any thoughts would be appreciated. The parents are at their wits end. He has also been treated with mupirocin cream in past with some success. Tacrolimus was not helpful.
The culture grew out coagulase positive staph sensitive to everything; even Penicillin G. This is unusual in the U.S. where most Saph is resistant to penicillin. One wonders if this is a strain he brought over from Russia when he was adopted. I started him on Pen VK 250 mg qid. I will add a topical corticosteroid and mupirocin - the latter for nares and crural folds. Will give follow-up after a couple of weeks. If he continues to have staph infections like this, I will look into his Ig status.
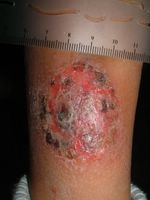
Right leg
This looks like impetiginous eczema, also known as nummular eczema, and is mainly caused by secondary invasion by staph aureus.
ReplyDeleteI agree - send pus for culture and sensitivity and this is almost always staph aureus. start him on oral flucloxacillin for at least 7-10 days. Daily dil. KMNO4 wash and moderate potency corticosteroids topically should help. Some would treat him with oral antibiotics for 2 weeks or even longer if it relapses frequently.
The whole picture is in favour of impetiginised discoid dermatitis which could be part of atopy or entity by itself.Regarding management,it is very essential to avoid all irritants like soaps,woollen clothes & with humid atmospher.Also KMNO4 wash with mixture of lococorten ointment and fucidin oinment topically plus oral seprin will be very helpful.
ReplyDeleteIt looks like infected discoid eczema.Generally they respond to a combination of a strong topical steroid and Mupirocin (Bactroban) creams.All the usual eczema admonitions have to be given to the patient but it tends to be recurrent.I have not had experience with Tacrolimus yet but Pimecrolimus would neither treat or prevent flares.
ReplyDeleteSurprisingly, I see many such cases in children throughout the year. Nummular eczema with superaded staph. infection would be a logical clinical diagnosis. My patients respond well to oral cefalexin or cefadroxil plus topical mupirocin and topical steroids. But the major problem remains the "recurrence of the lesions involving the same body sites" only a few months after complete clinical recovery. I do not have any experience with tacrolimus or pimecrolimus as these drugs are not available in Pakistan.
ReplyDelete