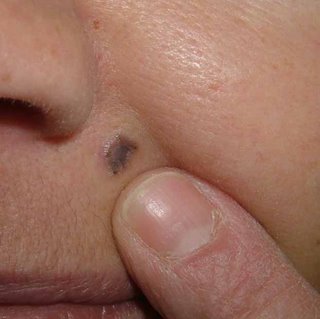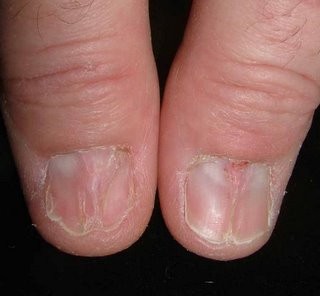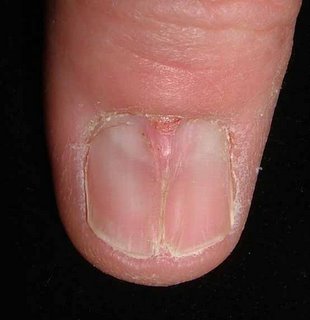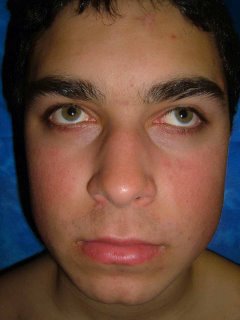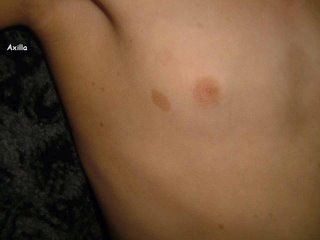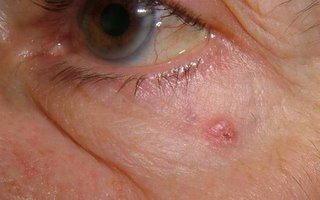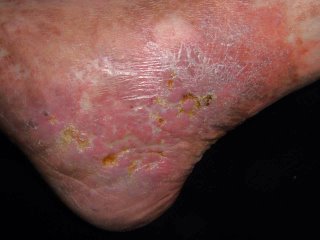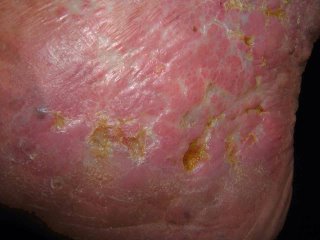
[Contents of Bag Brought in by Patient]
After a few years, he developed a febrile illness, was seen in the ER where a CBC showed a WBC of 80,000. He was eventually diagnosed with a rare T-cell lymphoma. Four courses of CHOP have put him in remission.
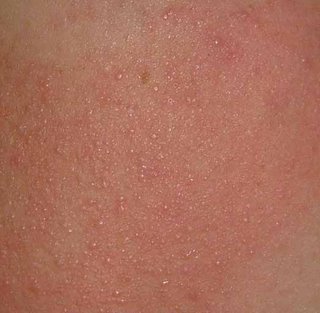
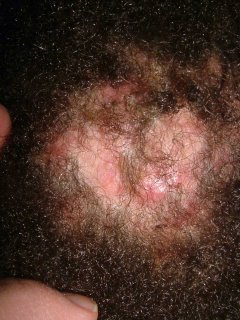
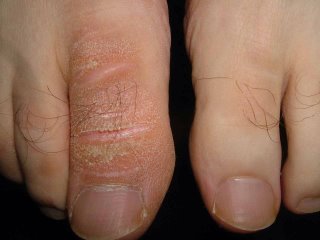
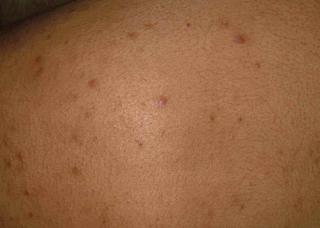
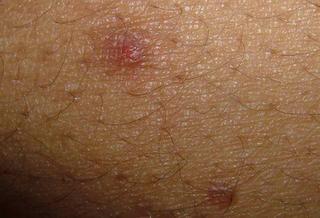
If his prurigo becomes more active again, one wonders if this will be a harbinger of recurrence.
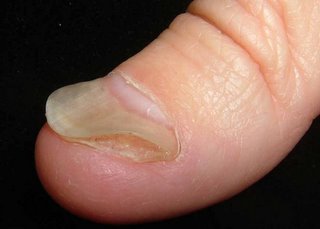
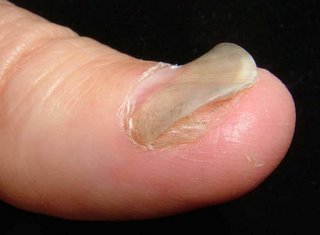
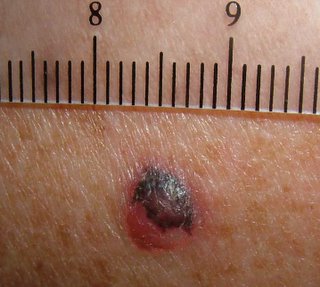
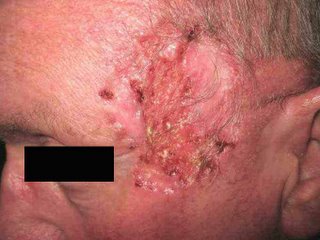
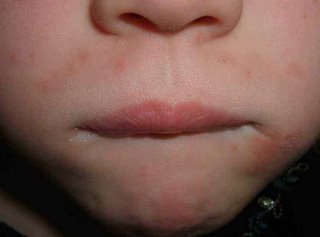
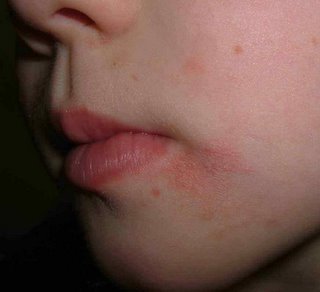
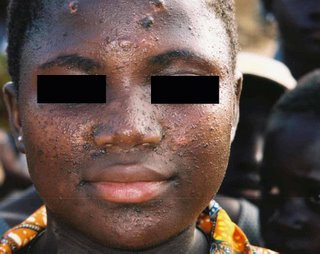
Sobering lesson. Prurigo may be realated to an underlying malignancy. We can all be lulled into a cream complacency and miss an important clue. I can think of one or two patients over the years with unexplained excoriations who turned out to have a lymphoproliferative malignancy.
Reference:
Seeburger J, Anderson-Wilms N, Jacobs R.
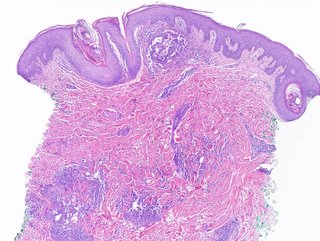
Lennert's lymphoma presenting as prurigo nodularis.
Cutis. 1993 May;51(5):355-8.
Section of Dermatology, Loma Linda University School of Medicine, California.
Abstract:
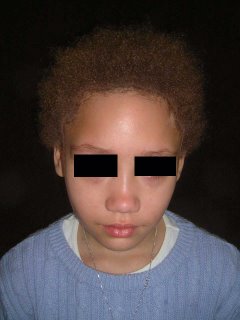
Lennert's lymphoma is a peripheral T-cell lymphoma that only rarely involves the skin. We present the case of a forty-two-year-old man who experienced severe pruritus for ten months. He was repeatedly diagnosed as having neurodermatitis
and prurigo nodularis before subtle hematologic clues suggested, and subsequent examination of bone and lymph node biopsy specimens confirmed, the diagnosis of Lennert's lymphoma. This report describes the case and presents a brief review
of Lennert's lymphoma.