Presented by Henry Foong, M.D.
Ipoh, Malaysia
The patient is a 80-year-old man who presented with swelling of the left leg for 3 months.
Ipoh, Malaysia
The patient is a 80-year-old man who presented with swelling of the left leg for 3 months.
About 3 years ago he had a motor vehicle accident where he injured his left leg. His attending doctor noticed a pigmented growth on the left foot associated with inguinal node swelling. A surgeon excised the pigmented growth on the left foot and removed some nodes from the left groin. No histological reports were available at the moment. The patient was well until recently when he noticed gradual swelling of the left leg with multiple pigmented nodules on the surface. The leg was occasionally painful at night. He did not have any constitutional symptoms. There was no family history of skin cancers. No significant other medical illness.
On examination his left leg was swollen and oedematous with many pigmented papules and nodules on the foot and lower 1/3 of the left leg. A pigmented ulcerating tumour 5 x 5 cm was noted on the left foot which extended to the heel. A firm matted lymph node swelling was noted on the left groin. There was a surgical scar over the left groin. No hepatosplenomegaly was present.
Biopsy of the pigmented papule on the foot was done and confirmed malignant melanoma.
Sheets and nests of malignant cells are seen invading the dermis. The tumour cells show marked pleomorphism, have increased nucleo-cytoplasmic ratio, vesicular nuclei with prominent nucleoli and eosinophilic cytoplasm. Many of the cells contain melanin pigment. Numerous mitotic figures are seen. The tumour is seen at the margins. Masson Fontana stain is focally positive.
Skin biopsy Report: Features are consistent with malignant melanoma.
On examination his left leg was swollen and oedematous with many pigmented papules and nodules on the foot and lower 1/3 of the left leg. A pigmented ulcerating tumour 5 x 5 cm was noted on the left foot which extended to the heel. A firm matted lymph node swelling was noted on the left groin. There was a surgical scar over the left groin. No hepatosplenomegaly was present.
Biopsy of the pigmented papule on the foot was done and confirmed malignant melanoma.
Sheets and nests of malignant cells are seen invading the dermis. The tumour cells show marked pleomorphism, have increased nucleo-cytoplasmic ratio, vesicular nuclei with prominent nucleoli and eosinophilic cytoplasm. Many of the cells contain melanin pigment. Numerous mitotic figures are seen. The tumour is seen at the margins. Masson Fontana stain is focally positive.
Skin biopsy Report: Features are consistent with malignant melanoma.
His work up included an oncology referral. CT scan of abdomen and pelvis which showed pelvic and para-aortic lymph
node metastasis. CXR normal. TWBC was 16,400. BRAF gene mutation studies pending
He was being treated for concomitant cellulitis with IV antibiotics.
Questions: What are the treatment options (targeted therapy) for his metastatic melanoma? Would oral vemurafenib and Anti PD-1 antibodies e.g. pembrolizumab be useful? They are very expensive though for most patients in Malaysia.
It's almost certain this patient will probably opt for palliative treatment. What local treatment of the in-trasit metastasis would be useful for him?
Thank you for your thoughts!
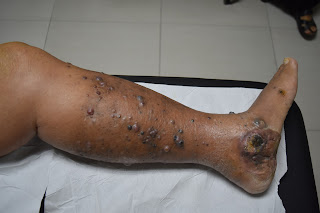


Dear Dr Foong palliative therapy is definitely required from the photos. Perhaps the BRAF gene status i.e V600E etc Mutation if known may help with possible choice / combination of checkpoint inhibitors. Also palliative radiotherapy ? Regards Dr C Tyson
ReplyDeleteSuch a difficult situation. Although we have drugs to treat metastatic melanoma, I think the side effects and of course cost would be prohibitive. There are a few dramatic cases of imiquimod creating a systemic response presumably through the effect of cytokines producing tumor regression locally and in distant mets. I also have a patient that has had 3 mets and is alive after 12 years. The mets in the lung and intestine were excised. I think that radiation could be helpful also to relieve tumor pressure on lymphatic.
ReplyDeleteFrom Mary Maloney, M.D. (micrographic surgeon): "I think that with biologic therapy, there is no reasonable therapy for this far advanced tumor. Radiation can be done for spot lesions but that is all.
ReplyDeleteHow sad."
from Patrick Kenny, Victoria, BC: Poor fellow has extensive intransit mets with nodal disease in pelvis and para aortic area . Older individuals are less likley to be BRAF positive , and if so response to vemurafinib is seen in maybe over 50% of cases but is short lived maybe 6 months before resistance seen. Are anti PD1 drugs available to you, this immunotherapy works frequently and a ongoing response seen if a significant percentage of patients. Cost is a hugh problem.
ReplyDeleteI have tried imiquimod 5 % cream in a somewhat similar case without pelvic disease used 5 nights per week with 5% 5FU used in am , initially with no occlusion then with plastic film occlusion for the imiquimod alone over night . After two years, all local disease was clear and she had no progression of the melanoma. Again one case
Wonder. Patient was in her 80's. Isolated limb perfusion and infusion used insome centres can do remarkable things but need specialized centre, and IL 2 injection used often now instead of melphalan infusion availble in one centre in Canada .