The examination shows a calm 9 year-old. Her scalp is involved globally with fluctuant nodules, some crusted. There are diffuse areas of alopecia. Some areas look scarred. Wood's light is negative. Posterior cervical lymph notes are enlarged and tender.
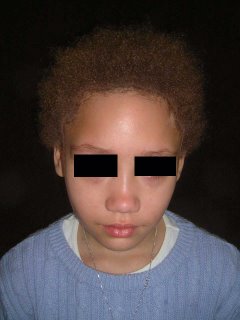
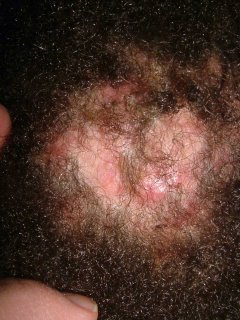
A bacterial and fungal culture were taken. Scalp biopsy will be performed and the patient will be started on prednisone 1 mg/kg/day and griseofulvin 25 mg/kg/day pending test results.
Working diagnosis is Inflammatory tinea capitis vs. dissecting cellulitis of the scalp.
Update February 9, 2006
The biopsies taken showed no fungfal elements, so the griseofulvin was discontinuted on Feb. 2, 2006 and patient was placed on cephalexin 50 mg/kg/day in divided doses. She did well.
On day 14, the fungal culture was positive and she was placed back on griseofulvin -- 25 mg/kg/day/ Her prednisone dose is 1 mg/kg/day.

Lesson: Scalp biopsy is not an absolute. Fungal culture takes ~ 2 weeks to be positive.
Dx: Inflammatory tinea capitis (the first diagnosis). Negative scalp bx threw me off.
Your comments are welcome.
Reference:
Tinea capitis mimicking dissecting cellulitis: a distinct variant.
Twersky JM, Sheth AP.
Int J Dermatol. 2005 May;44(5):412-4.
BACKGROUND: Tinea capitis is a common scalp dermatosis with several clinical
patterns. Only two patients with a presentation of tinea capitis mimicking
dissecting cellulitis have been described in the English literature.
OBSERVATION: We report a patient with tinea capitis mimicking dissecting
cellulitis who did not respond to griseofulvin therapy at 16 mg/kg/day but
eventually cleared after a protracted course of higher dose griseofulvin.
CONCLUSION: recognition of a dissecting cellulitis-like pattern of tinea capitis
will increase clinical suspicion and avoid inappropriate management of a
recalcitrant "dissecting cellulitis" in favor of prompt antifungal therapy of
appropriate dosage and duration for patients with this unusual variant of tinea
capitis.
I would favour dissecting cellulitis of the scalp vs inflammatory kerion of tinea capitis. Another differential that need to be considered include lupus erythematosus and folliculitis decalvans. Biopsy and bacterial culture would all help. Staph aureus is most likely to be isolated from such culture. Rifamipicin and another anti staph antibiotic ( eg cloxacillin or fusidic acid) would be a useful combination. I think intra lesional corticosteroid would be useful for the inflamed alopecic areas.
ReplyDeleteHenry